The Shoe Finally Dropped
You know when things are going well and you are just waiting for something bad to happen? That has been how I've felt for the past couple of weeks. Each time a doctor or nurse would tell me how great Finn is or how well he's doing I paused for the "but." I was waiting for the other shoe to drop.
The last four days have been in competition for the worst of my life. I don't even know where to start with processing what my sweet boy has gone through. No child, no baby, should ever have to endure the trauma that Finnegan has experienced. My whole body aches for him. Prior to Sunday night I was told regularly how my son was a rockstar on ECMO, he was void of any traditional complications. At each comment I would look at the doctors or nurses with fear in my eyes because I knew at any moment it could change.
On Sunday Finn seemed pretty normal, relative to his condition. He was happy and active. We played and my mom came to visit. I had my typical anxiety leaving that evening but for the most part things seemed fine. Halfway through my drive home I had a wave come over me. My palms got sweaty, my mouth watered and my heart sank to my stomach. I sent Jeff a text asking how Little was doing. Instead of his traditional text response, he called. He couldn't believe how I knew something was wrong. Finn's incision, where the cannulas are placed, was oozing and they would need to sedate and redress. Blood loss is common and dangerous for Finn's condition. He has to be on a lot of anticoagulants to keep his ECMO circuit clean. Clots are dangerous if they get loose and enter his body. On the other hand, not clotting could lead to blood loss or internal bleeding. Each day it's a balance. No clots, no bleeding.
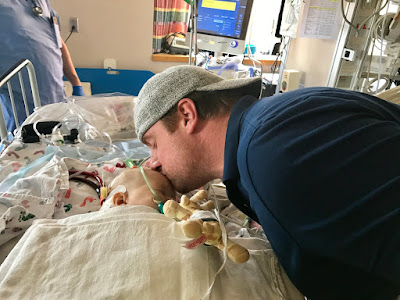
Then, on Monday Jeff sent me a picture. Finn was grey. The difference between the child I left on Sunday and the child he sent a picture of was dramatic. His cannulas, the ones that are directly placed in his carotid and jugular came out of position. Finn needed to go to the operating room to get them placed properly. I was at work when Jeff told me. Immediately I stood up in the middle of my meeting and ran out in tears. I had to get to Rochester, fast, so I could kiss my baby before his procedure. At 3:27 PM they took him for his first trip outside ICU room 14 in 35 days. I was told that he had his eyes open and was enjoying looking around while he felt the movement of the bed rolling down to the OR.
Finn's procedure went well. They were able to reposition his lifesupport so that he was getting optimal profusion to his major organs. He was safe. When he came back to us he was highly sedated and still intubated but the doctors were optimistic that they would be able to get him off the ventilator. By 10:30 PM that evening he was freely breathing on his own without support. He was pink again and seemed more himself. Then, on Tuesday morning he was put on CPAP support. He just wasn't able to keep his lungs clear on his own. This wasn't completely unexpected as last time he was extubated he struggled for a few days as well. By Tuesday afternoon he was able to take breaks from the mask and participate in his music therapy. Finn loves watching the therapists play and sing to him. He seemed content but not back to himself by any means.
Tuesday night Finn refused to settle in. He was grunting, wiggling and overall could not get himself to a restful state. It was so much to the point that I actually asked our nurse, Blake, if he could have additional sedatives. Now, this is impressive because I am not one to default to medical treatments or sedatives. We had just worked so hard to wean him down. But, he needed it. It was past 1:00 AM and I was exhausted. Nothing I could do would help him calm down.
Early Wednesday morning I walked into our room and saw the grey twin of my sweet Finn, again. Listless, grunting and unresponsive. He didn't even protest to his diaper being changed or the removal of his blankets. Something was definitely wrong. All day I would tell anyone who listened that he wasn't my baby. I cried. He was so different. Finally late Wednesday night after he didn't wake up to his bath Dr. Schears took action. We played with his CPAP settings, tried BIPAP, CPT and other ways to get him to clear his lungs. They couldn't catch any movement while listening to him. There was fear that his lung was collapsed. We had to think about intubating.
After an hour of trying different things and getting no positive response, the call was made. Quickly 10 people, nurses, Dr. Schears, PA, RTs and other support staff members were swarming our room. They began bagging him, manually pushing air into his lungs. Almost immediately breast milk and gastric fluids poured out of his nose and mouth. Our nurse, Lisa, had cleared his stomach prior to the call for intubation being made. Where was it coming from? They suctioned, over and over and over again. Bag, suction, bag, suction. Finally Dr. Schears went to intubate. He successfully placed the breathing tube the first time. More suction and then he was on the vent. Almost immediately his lips went back to pink. The whole process was a few hours from when we first started to try and recuperate some of his lung function to him resting more comfortably. The did a bronchoscopy to be sure the tube was above his carina appropriately. Last time he was right mainstem and we didn't want that. On the screen you could see that he was raw. That there was some slight bleeding. Bleeding, on ECMO is terrifying.
I didn't sleep at all that night. I was so scared. Finn had been doing well up until this. No real complications from his ECMO. It's a great run, 42 days, but we still have many to go while we wait for our heart. His cultures came back positive. MSSA was found in both his broviac line and the ECMO. Sepsis. Most people who die waiting for an organ pass not because of their organ disease but because of infection or illness. Not only that, but having an infection could make Finn ineligible to receive his life saving gift if it came. Dr. Johnson, our cardiologist, told me it would be a game time decision if we got the call. He said that he wouldn't go and get a heart, but if one was a perfect match and coming from Mayo he would think about it. The tears poured out. Was this it? Would this be what took my son from me?
Finn had already started on antibiotics so we were hopeful that they would take care of the infection and fast. They also had to take ET tube secretions and test them for pneumonia. Additionally, each time they suction him they are pulling up blood. Blood is scary. He is on a heavy dose of blood thinners to keep the circuit from clotting, which means he can't clot either. The whole ECMO game is a balance. Increase the blood thinners so that the circuit doesn't clot and the risk of internal bleeding goes up. Turn the blood thinners down so that he can clot and the circuit gets junky. If one of those clots gets loose and into our sweet boy, he could have a stroke. Right then we needed him to stop bleeding from his carina so that the blood doesn't start pooling into his lungs and inhibit his ability to produce oxygen. Dr. Van Dorn made the call to reduce the bivalrudin to half it's dose. We needed the bleeding to stop. For the rest of the day the team had to inspect the circuit every hour rather than every four. The nurses had to be extremely judicious on when to suction out his secretions so as not to irritate the rawness of his trachea. Along with this dance we had to balance his level of sedation after finally getting it to a manageable point. Not too much as to completely knock him out, but enough to keep him comfortable so he doesn't hurt himself. After all that work to wean him we were back to finding a new balance.
Yesterday felt better than the days prior but not as good all the days leading up to it. His head ultrasound came back normal and his kidneys appear to be doing their job. They took more labs to see if the infection had cleared but now his hemoglobin was getting low. Blood transfusions are common on ECMO but unfortunately very bad for transplant patients. The more transfusions the more antibodies you enter into the equation. The more antibodies, the more likely rejection is to occur when he gets his new heart. Finn has had half a dozen transfusions to date. Currently he is sitting at a very low hemoglobin (7.4) and we are holding out as long as we can.
When I came into the hospital today Finn was resting. The culture from his broviac had come back negative so far (yay!) but the culture from the circuit was positive. Which means, the infection is lingering somewhere on the hardware. Now we have to see if we can kill it there too. First we will up or change the antibiotics but if that doesn't work he will likely need a new ECMO circuit. The risks are substantial with changing out the circuit and this will be his fourth time. Each time the risks go up.
Dr. Johnson shared news with me last night that a young man who was hospitalized since December last year was receiving his gift. He wanted me to know so that I wasn't surprised when there was a lot of commotion and talk of transplant on the unit. He seemed concerned that I would be upset it wasn't Finn's heart he was telling me about. My knees got weak and I collapsed onto my son's bed. I wasn't able to form words. Right now I can't even type this without tears streaming down my face. He is saved. A child here at Mayo is going to live because someone made the difficult decision to honor their little one by saving someone else. I was elated, and sad. Scared and hopeful. There were no feelings of jealousy or resentment that it wasn't Finn's turn. Just darkness for the family who had lost their baby and light for the family who will be able to someday soon take theirs home after seven months of wait.
Right now my son's heart, the one that he needs, is still beating in another child's chest. Another baby requires it more than Finn today. Another mommy still needs her baby and right now mine is okay. On lifesupport, but okay.
June 9th, 2017
The last four days have been in competition for the worst of my life. I don't even know where to start with processing what my sweet boy has gone through. No child, no baby, should ever have to endure the trauma that Finnegan has experienced. My whole body aches for him. Prior to Sunday night I was told regularly how my son was a rockstar on ECMO, he was void of any traditional complications. At each comment I would look at the doctors or nurses with fear in my eyes because I knew at any moment it could change.
On Sunday Finn seemed pretty normal, relative to his condition. He was happy and active. We played and my mom came to visit. I had my typical anxiety leaving that evening but for the most part things seemed fine. Halfway through my drive home I had a wave come over me. My palms got sweaty, my mouth watered and my heart sank to my stomach. I sent Jeff a text asking how Little was doing. Instead of his traditional text response, he called. He couldn't believe how I knew something was wrong. Finn's incision, where the cannulas are placed, was oozing and they would need to sedate and redress. Blood loss is common and dangerous for Finn's condition. He has to be on a lot of anticoagulants to keep his ECMO circuit clean. Clots are dangerous if they get loose and enter his body. On the other hand, not clotting could lead to blood loss or internal bleeding. Each day it's a balance. No clots, no bleeding.
Then, on Monday Jeff sent me a picture. Finn was grey. The difference between the child I left on Sunday and the child he sent a picture of was dramatic. His cannulas, the ones that are directly placed in his carotid and jugular came out of position. Finn needed to go to the operating room to get them placed properly. I was at work when Jeff told me. Immediately I stood up in the middle of my meeting and ran out in tears. I had to get to Rochester, fast, so I could kiss my baby before his procedure. At 3:27 PM they took him for his first trip outside ICU room 14 in 35 days. I was told that he had his eyes open and was enjoying looking around while he felt the movement of the bed rolling down to the OR.
Finn's procedure went well. They were able to reposition his lifesupport so that he was getting optimal profusion to his major organs. He was safe. When he came back to us he was highly sedated and still intubated but the doctors were optimistic that they would be able to get him off the ventilator. By 10:30 PM that evening he was freely breathing on his own without support. He was pink again and seemed more himself. Then, on Tuesday morning he was put on CPAP support. He just wasn't able to keep his lungs clear on his own. This wasn't completely unexpected as last time he was extubated he struggled for a few days as well. By Tuesday afternoon he was able to take breaks from the mask and participate in his music therapy. Finn loves watching the therapists play and sing to him. He seemed content but not back to himself by any means.
Tuesday night Finn refused to settle in. He was grunting, wiggling and overall could not get himself to a restful state. It was so much to the point that I actually asked our nurse, Blake, if he could have additional sedatives. Now, this is impressive because I am not one to default to medical treatments or sedatives. We had just worked so hard to wean him down. But, he needed it. It was past 1:00 AM and I was exhausted. Nothing I could do would help him calm down.
Early Wednesday morning I walked into our room and saw the grey twin of my sweet Finn, again. Listless, grunting and unresponsive. He didn't even protest to his diaper being changed or the removal of his blankets. Something was definitely wrong. All day I would tell anyone who listened that he wasn't my baby. I cried. He was so different. Finally late Wednesday night after he didn't wake up to his bath Dr. Schears took action. We played with his CPAP settings, tried BIPAP, CPT and other ways to get him to clear his lungs. They couldn't catch any movement while listening to him. There was fear that his lung was collapsed. We had to think about intubating.
After an hour of trying different things and getting no positive response, the call was made. Quickly 10 people, nurses, Dr. Schears, PA, RTs and other support staff members were swarming our room. They began bagging him, manually pushing air into his lungs. Almost immediately breast milk and gastric fluids poured out of his nose and mouth. Our nurse, Lisa, had cleared his stomach prior to the call for intubation being made. Where was it coming from? They suctioned, over and over and over again. Bag, suction, bag, suction. Finally Dr. Schears went to intubate. He successfully placed the breathing tube the first time. More suction and then he was on the vent. Almost immediately his lips went back to pink. The whole process was a few hours from when we first started to try and recuperate some of his lung function to him resting more comfortably. The did a bronchoscopy to be sure the tube was above his carina appropriately. Last time he was right mainstem and we didn't want that. On the screen you could see that he was raw. That there was some slight bleeding. Bleeding, on ECMO is terrifying.
I didn't sleep at all that night. I was so scared. Finn had been doing well up until this. No real complications from his ECMO. It's a great run, 42 days, but we still have many to go while we wait for our heart. His cultures came back positive. MSSA was found in both his broviac line and the ECMO. Sepsis. Most people who die waiting for an organ pass not because of their organ disease but because of infection or illness. Not only that, but having an infection could make Finn ineligible to receive his life saving gift if it came. Dr. Johnson, our cardiologist, told me it would be a game time decision if we got the call. He said that he wouldn't go and get a heart, but if one was a perfect match and coming from Mayo he would think about it. The tears poured out. Was this it? Would this be what took my son from me?
Finn had already started on antibiotics so we were hopeful that they would take care of the infection and fast. They also had to take ET tube secretions and test them for pneumonia. Additionally, each time they suction him they are pulling up blood. Blood is scary. He is on a heavy dose of blood thinners to keep the circuit from clotting, which means he can't clot either. The whole ECMO game is a balance. Increase the blood thinners so that the circuit doesn't clot and the risk of internal bleeding goes up. Turn the blood thinners down so that he can clot and the circuit gets junky. If one of those clots gets loose and into our sweet boy, he could have a stroke. Right then we needed him to stop bleeding from his carina so that the blood doesn't start pooling into his lungs and inhibit his ability to produce oxygen. Dr. Van Dorn made the call to reduce the bivalrudin to half it's dose. We needed the bleeding to stop. For the rest of the day the team had to inspect the circuit every hour rather than every four. The nurses had to be extremely judicious on when to suction out his secretions so as not to irritate the rawness of his trachea. Along with this dance we had to balance his level of sedation after finally getting it to a manageable point. Not too much as to completely knock him out, but enough to keep him comfortable so he doesn't hurt himself. After all that work to wean him we were back to finding a new balance.
Yesterday felt better than the days prior but not as good all the days leading up to it. His head ultrasound came back normal and his kidneys appear to be doing their job. They took more labs to see if the infection had cleared but now his hemoglobin was getting low. Blood transfusions are common on ECMO but unfortunately very bad for transplant patients. The more transfusions the more antibodies you enter into the equation. The more antibodies, the more likely rejection is to occur when he gets his new heart. Finn has had half a dozen transfusions to date. Currently he is sitting at a very low hemoglobin (7.4) and we are holding out as long as we can.
When I came into the hospital today Finn was resting. The culture from his broviac had come back negative so far (yay!) but the culture from the circuit was positive. Which means, the infection is lingering somewhere on the hardware. Now we have to see if we can kill it there too. First we will up or change the antibiotics but if that doesn't work he will likely need a new ECMO circuit. The risks are substantial with changing out the circuit and this will be his fourth time. Each time the risks go up.
Right now my son's heart, the one that he needs, is still beating in another child's chest. Another baby requires it more than Finn today. Another mommy still needs her baby and right now mine is okay. On lifesupport, but okay.
June 9th, 2017






Comments
Post a Comment