Friday the 13th
When the nurse said I should think about putting together a Caring Bridge site, I lost it. Only sick people have Caring Bridge pages and my baby is going to get better. He was only supposed to be here for 24 hour monitoring due to a little extra fluid in his lungs. How are we still here and how did it go from a beautiful and unexpected home birth to me crying by my fragile son’s bedside in the NICU with more questions than answers?
This isn’t a Caring Bridge, this is my story. Our story. Finnegan’s Journey into this world.
My pregnancy with Finn was so different than Asher. From the beginning I had different symptoms including incredible fatigue and morning sickness all the way into the middle of my pregnancy. With Asher, I only had breast tenderness and that went away at 12 weeks on the day. Other than that, I felt amazing (with a little side of heartburn). Being pregnant with a toddler was a whole new experience. All the literal ups and downs of lifting, squatting, crawling, running, playing and cleaning up on top of a growing belly and fatigue was a challenge. Throughout my pregnancy I felt guilty for not enjoying it as much as I did last time, but I knew that the reward that waited for me on the other end would be worth it.
Pregnancy changed me. It opened my eyes to how everything you put in and on your body can impact another human. I eat organic, whole foods whenever possible. I exercise regularly, use non-toxic plant based self care items and stay away from plastics and dyes. None of that was making it anywhere near my body or my children’s. I have this whole “health” thing nailed. Right? As Jeff recently reminded me, “We don’t have as much control as we think we do.”
On Friday January 13th I was attending the funeral of someone that I care deeply about. A mother and grandmother who passed away somewhat unexpectedly the week prior. It was the day before my “guess” date and I had been having a few signs of my impending labor, nothing too serious. As I hugged her husband and shared my condolences I felt my water break. Here we go! I rushed to the bathroom with the help of a friend. When I got to my car I headed home and called my husband, midwives, mom and doula. It was time. We waited for contractions to start. Resting, eating and trying not to get too excited. Jeff picked up Asher from school and my mom came over to play while we labored at home as long as possible. The first few hours passed rather quickly. Still playing and talking through contractions. Once I started to feel the need to moan through them I went in my bedroom with relaxing music, essential oils and candles lit. Jeff rubbed my back and assured me that I was amazing. He kept telling me what a wonderful mother I am and how proud of me he is. We can do this!
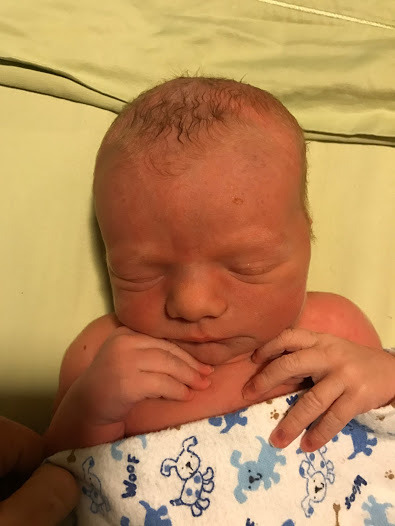
After a few check ins with my midwives and doula things started to really turn up. Around 7:30 contractions were getting far more intense, maybe we should head into the birth center. My midwife needed a half an hour to get there. Our doula was on her way to the house. The plan was to meet right around 8 PM. At 7:51 PM I sent a text to my doula saying “maybe we should meet at the birth center rather than home” and Jeff went to heat up the car. The contractions were getting so hard and coming so fast. I went to go to the bathroom before and screamed for Jeff to come in. I could feel the head! I don’t think we are going to make it to the birth center. Jeff quickly called our midwife and our doula showed up throwing off her jacket and running into the bathroom falling to her knees. “We have a head!” I heard Jeff say. My doula was calm and in constant communication with our midwife on speaker phone. She made a comment about one push to get the shoulders out and he fell right into her arms. She lifted him on to my chest and Jeff proclaimed “It’s a boy! Another boy!” He was here. In my arms In my bathroom. I have never felt so powerful. Proud, strong, happy, secure. In love. Here my son came into my arms in the comfort of his own home. A bit like a whirlwind, but also peaceful in a way. We were already home and safe. Our midwife and nurse showed up 10 minutes later and we assessed our boy, let the cord stop pulsing and started to gather ourselves together.
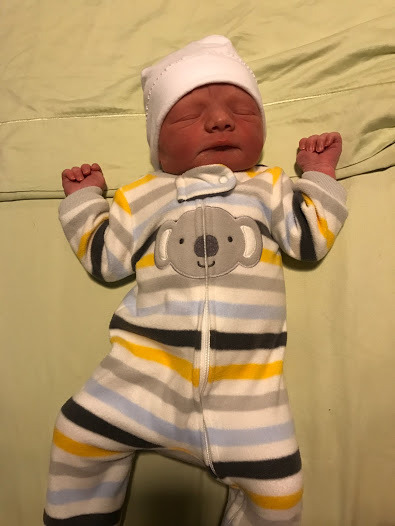
They moved me to my bedroom and started afterbirth care for me and our son, Finnegan Moore Olson. We snuggled and snuggled. He latched perfectly. It was heaven! I had never thought about or planned on a home birth but I could see why someone would wish to have their children at home. Shortly after we were comfortable and snuggled in Asher came in to meet his brother. “Thats my baby, I am big!” This was perfection. A safe and healthy birth in the comfort of my own home. We don’t have to go out into the cold. Mmmm, new baby smells and sounds.
After several checks and re-checks, Finn’s oxygen levels weren’t matching on his hand and his foot. Our midwife told us that means his heart may not be pumping blood through his body properly. That coupled with some labored breathing means he may have some fluid still in his lungs. Nothing to worry about, Transient Tachypnea of the Newborn (TTN) is pretty common with children who are born so quickly. We should probably go to Children’s Hospital and be monitored. They may keep us up to 24 hours but we will be home before we know it. There goes my birth plan once again. Hospitals were never in this equation. But, we need to get him checked. We packed up Finn and an overnight bag and headed to Children’s in Minneapolis around 2 AM on Saturday, January 14th.
We arrived at the Hospital and were pre-checked for the Specialty Care Nursery. We got settled and the doctors and nurses started hooking him up to monitors. They wanted to start him on antibiotics just in case it was pneumonia or another infection in his lungs. This was before they even looked at his lungs, just based on listening. I was confused. We have to start treating him for something that he may or may not have? Can’t we assess him first and then determine treatment based on what we find out? It seemed a lot like “fire, aim, ready” and my programatic problem solving brain doesn’t quite work that way. I cried so hard. His body is so new and we are going to pump him full of antibiotics and Dextrose. They want to expose him to x-rays and poke his little body for IVs and lab work. How did we go from a med-free birth plan to a medically induced nightmare?
After a day of rising and falling oxygen levels and labored breathing the nurses finally decided to put him on oxygen to see if that helped his little lungs. The grunting noises started to dissipate and he seemed to be doing better. His sugar levels were getting higher and he was still nursing well. We were weaning off the Dextrose. I asked when we would be able to go home, the answer was as early as Monday or as late as a week. It just depended on getting back his infection reports and when we could take him off the antibiotics. I continued to nurse him on demand and we snuggled as much as we could. Jeff had to travel back and forth to help my mom with Asher so I stayed with Finn.
Sunday January 15th we had a follow up x-ray to see how his lungs were clearing out. Unfortunately, no change. They still looked wet and dark. He wasn’t absorbing the fluid like a child with TTN would. All of the infections that they tested him for were coming up negative. The Nurse Practitioner on staff listened to his heart and brought in a doctor. He said the whooshing noise was getting louder and the hole that was supposed to be closing after birth didn’t seem to be doing what it’s supposed to. We need to do an Echocardiogram. At this point, I was so lost. They have now treated and ruled out so many different issues. Why do we keep acting first and then diagnosing after? My poor boy has been through so much.
After the Echo everything happened so fast. Jeff was home taking care of Asher and I was alone in Finn’s room. The sweetest nurse, Margaret, came and sat down with me. She had noticed that I hadn’t slept or eaten and she brought me a protein shake, a Lara Bar and a bag of nuts. She forced me to eat. When I had finished the protein shake she put her arms around me and told me that the Cardiologist was on his way down. I asked her if that meant that it was bad news. Margaret then told me that they were moving Finn to the NICU. Clearly it wasn’t a good sign. She didn’t know anything else, just that I had to pack up and head up to Finn’s new room on the 3rd floor.
Shortly upon arriving in our new room in the NICU we were introduced to the Neonatologist and Cardiologist on shift. They started talking and I couldn’t hold back any more. Weren’t we just coming here for a quick monitoring of his breathing while his lungs worked to absorb the amniotic fluid? Now we are surrounded by doctors and nurses talking about our little baby’s heart. They started by telling us that Finn’s heart is too big. Hypertrophic Cardiomyopathy (HCM). His left ventricle is enlarged and isn’t working properly. The tissue is too hard and therefore it can’t pump the way it should. I can’t remember all the parts and pieces and what they are supposed to do but I tried to follow along. They quickly start talking about taking tests, lots of tests. There are any number of things this can cause this but they have something called Pompe Disease at the top of their list. The next step is for him to get a lot of blood and urine drawn and to send it off to the Mayo Clinic and Duke University. A Geneticist will be in to talk to us about it more.
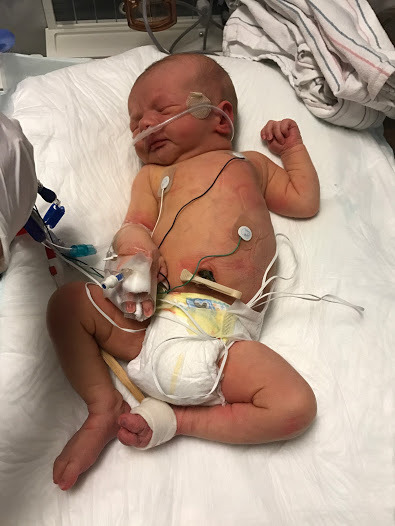
A disease? My world just flipped upside down. They didn’t tell us what this disease meant, just the name of it and how it works. Glycogen storage, floppy baby, feeding tubes, breathing help and muscle weakness, an enlarged heart. Just a few of the pieces that I could follow. They had to work quickly to get in internal line into his umbilical cord stump so they could take blood without pricking him over and over again and send it out. Jeff was back in time to hear all of this and we were ushered out of the room so they could start the process. We did exactly what anyone did at this point. We Googled Pompe Disease. It was the only name that they gave us. They said it could be Pompe or any number of other things. Pompe, Pompe, Pompe. I asked about their level of certainty and they remained objective just as you would expect. Googling the disease made me die a little inside. The outcomes are not good. Especially for a child Finn’s age. Life expectancy and quality of life are not what I would qualify as “okay” by any means. My head was flooded with thoughts of the future. All the opportunities and events that our sweet boy would miss out on. How do you find hope in this situation?
When the procedure was done to set the internal lines we went back in our room. We have another child we still need to care for. Do we stay here with Finn or go home to Asher? Finn was no longer able to nurse, they wanted him to concentrate on breathing so they were inserting a feeding tube. I had some pumped milk for him, enough to get him through a couple of feedings. We decided to head home and try to provide Asher with some sort of “normal” for the evening. Finn was resting comfortably and was in the stellar care of the adoring NICU nurses.
Home was supposed to feel good. It was supposed to feel safe and “normal” after being in a hospital for the past few days. But, it didn’t. Asher wasn’t excited to see me and was busy playing with my mom. Jeff and I were broken and didn’t know how to act “normal.” I needed a shower and just a minute alone to process my thoughts. I went into my bedroom and fell apart. How is my perfect little boy not home with me? He was born here at home, he is not supposed to be at the hospital. This is not the way it should be. My biggest problems should be balancing a two year old and the sleep deprivation that goes along with having a newborn. This is not my life. This is not what Finn’s life is supposed to be like. I pulled myself together long enough to make it to the bathroom. The bathroom where Finn was born. I collapsed. Is that why he was born here? So that he could meet his brother and be home at least once? Was he ever going to come home again? So many questions and unknowns. So much fear and anger. I don’t know how long that shower lasted, but I know I wailed louder and harder than I ever have in my life. I have never known a pain like this. I need to take Finn’s hurt away. I have to save him from this terrible outcome. I can’t.
Monday January 16th, 2017 was MLK day and Asher was off school so my mom continued to help us. I was with Finn all day again. Throughout the day there was a series of people coming through a rotating door in our room. The Neonatologist, Cardiologist, Geneticist, Social Worker, Child Life Specialist, my Midwives and nurses all came by. Each one with a different set of information or questions. My head was spinning. I asked a lot of questions. They talked a lot. We talked about Finn, Pompe, how to be a “NICU Family” and take care of Asher, what my options were for parking, Ronald McDonald House, how to tell Asher what is going on, tests and results and when to expect them and so much more. Because Jeff was still home taking care of Asher I was trying to communicate everything back to him that I could. There was so much to take in. This is our new life. At least our new life for the immediate future. If Finn has Pompe disease he will need Enzyme Replacement Therapy (ERT) and will be in the hospital for at least a month or two depending on how he tolerates it. This could be our life longer term. Jeff finally came and it was lunch time. The visits didn’t stop and we continued to be flooded with information.
At 4 PM we decided to head home to have dinner with Asher and put him to bed. I would come back and sleep at the hospital again with Finn, but not until Asher was down. Trying to be “normal” or at least appear that way for Asher. As we stepped out of our room our lovely nurse, Liz gave us a high-five and said “good day guys!” Ummmm, what? That was a “good” day? I mean, yes his stats all remained stable most of the day and we got to hold Finn more than the day previous but I didn’t consider this “good” by any means. Is this now what a good day is going to look like for our family? I died a little more. I need to start readjusting my expectations.
The Social Worker had told me that I need to make a plan and schedule for the first week. How do we get to the official diagnosis? I decided that I will split my day between home and the NICU. During the day while Asher is at school I will be with Finn. Pumping, snuggling, reading to him and loving on him. Then I would pick Asher up from school and have dinner, play and bedtime. After that, back to the hospital to spend the night with Finn again. I can do this. At least until diagnosis.
On Tuesday morning I arrived home before Asher and Jeff woke up. I showered and pumped and we got Asher ready for school. I let his teachers know the high level situation. Finn is in the NICU and we don’t know how serious it is. Asher had bizarre weekend and may be a little “off” of his schedule. We asked that they please keep an eye on him and report back if there was anything unusual in his behavior. We also provided them with language on how we are talking about Baby Finn so we are consistent across all of the adults in his life. Back to the hospital we go.
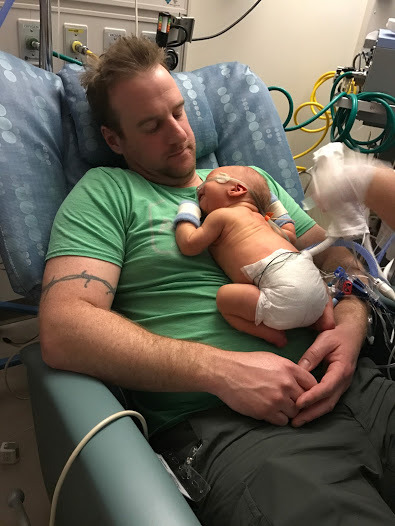
More snuggles. Skin to skin. I inhale deeply the sweet smell of newborn. I can’t stop kissing his little head. Isn’t it funny how newborns look like little old men? He sort of looks like Papa. Oh how I love this little nugget. How can he be sick? He looks so perfect on the outside. How does his little heart not work properly? The nurse who was on duty when we came back had taken him off the heater and said his respirations had been on track since. When the Neonatologist came in he said that Finn was doing great. That his stats were all where they were supposed to be and if he could keep his respirations in the right range for 24 hours we could try to do oral feeds on Wednesday. I cried, this time out of a little glimmer of happiness. I have been slaving on the pump to provide milk for my little boy and missing all the normal ways I know how to be a mother. I haven’t changed my child’s diaper or nursed him since Sunday. I haven’t been able to pick him up when he cries or rock him to sleep. Now, there was a little hope that I may be able to do one of these things. Something that was so important to me. The little wins have to be celebrated at this point. Hold on to this, for now.
Jeff and I went to lunch later in the day. We walked, mostly silently, holding onto one another through the mile long tunnel system to Midtown Global Market. I haven’t had chips and salsa for so long. Let’s go do that. We didn’t really have too much to say. We are angry, scared, sad, nervous and already grieving. After lunch, we head back for more snuggles and to spend time talking to Finn while the clock ticks down and we need to pick up Ash. We start to talk about life expectancy and quality of life again but it’s just so hard to go there. Pompe is the enemy we are fighting and we are being told it is our most likely outcome. How do you prepare yourself for something like this?
The Geneticist knocks on the door and enters our room after lunch. He has an update. Not all the labs have come back yet, and there have been a lot of negative results. We have one definitive answer. Finn has a Carnitine Deficiency. He explains it as a truck that carries a protein down a highway. Finn’s truck doesn’t work and so the protein isn’t making it’s way to the parts of the body that it’s needed. Therefore there is a sort of scar tissue building up in his heart causing the enlargement. There are two forms of CD, Primary and Secondary. If it’s Primary it could be the only thing wrong with him and treated easily with an oral or IV supplement. If it’s Secondary it likely is coupled with something else that will need to be looked at. The first step is to test me, because I would be the one who passed it on to him in gestation. I could have a Carnitine Deficiency and not even know it. Of course, our first question is back to Pompe Disease. He shared with us that the symptoms are very similar. There is no direct correlation between CD and Pompe, but that doesn’t mean he can’t have both. We won’t know until we get definitive Pompe results. In the meantime we can immediately start giving Finn the supplement for CD.
What is this feeling? Is it HOPE? Something that I felt like was so lost. Each doctor we spoke with seemed convinced that Pompe was our outcome. They told me to prepare for the worst. That it’s “at the top of the list” of and that all signs point to Pompe. Now, we have at least one small answer pointing to something other than Pompe. Again, it doesn’t mean he can’t have both. But what is the likelihood that he has two different conditions that each have the exact same symptoms? I don’t want to get too hopeful. Can I let myself go there? We still don’t know all the results and may not for days or even a week. But, if this is what is wrong with Finn it’s treatable and he can have a normal life. It’s a glimmer and I am going to hold on to it with everything I am.
The Geneticist was the first one to start talking numbers to us. Today was the first time we had heard that 50% of people with Cardiomyopathy go undiagnosed because they can’t even figure out why it happened. The other 50%, they can assess and diagnose. Of that 50%, 10-15% with this sort of heart enlargement (specific to the left ventricle) end up with Pompe so that is the reason they have it at the top of his list. Wait. The reason it’s at the top is because of a percentage? Here we thought it was the top of the list because of FINN and the way he was presenting. Now I am more hopeful. Should I be? For today I am going to hang on to the hope and light. For today I am going to go home and hug Asher and think that maybe our Baby Finn will be coming home to stay. That “normal” is still achievable. The orders for his Levocarnitine are in and he will start on the medication immediately. They will take another look at his heart in a week and see if there is any visible improvement. Maybe tonight I will sleep…
January 17, 2017







Comments
Post a Comment