"Danger" is My Middle Name
When I was pregnant with Finnegan we nicknamed him Danger. It popped up when I was searching for baby names one day and we thought it was hilarious. Would anyone really contemplate naming their child Danger? Every week when I would get my pregnancy updates it would say “Danger Olson is the size of a cantaloupe” or whichever fruit was comparable to my sweet boy’s growth. It always gave me a laugh.
-
Finn had a tough weekend. He lost his NJ tube, twice, and had a hard time recovering from the stress he went through to get it replaced. Then early Sunday morning he was quite sweaty and his PICC line slipped out. All relatively small things, however his heart condition doesn’t give him much reserve energy to be stressed out. He was clearly agitated, crabby, sweaty and tired. Not the sweet child we saw smiling and playing the week prior. Since he was born I have always been able to console him. By Monday and Tuesday even my touch wasn’t doing the trick.
Between losing his PICC line, NJ tube and our inevitable trip to Mayo for eventual listing, our team decided that Finn was going to require more permanent accessories. The planned to place a Broviac line and GJ tube on Wednesday. Of course, as always, I was upset but knew it was what is best for him. I was terrified because he has not been sedated yet and to do the procedures they need to intubate him. Sedation comes with risks for anyone, let alone my brand new baby with a severe heart condition. My fear was valid. At least I had time to plan and process things. Right?
Finn is impatient. I should’ve known by his speedy entry into the world. This kid wants to be early. Not too early, but definitely before we are ready for him. On Tuesday Dr. Rood called me at work and shared that he was having some significant work of breathing and she wanted to give him additional help. They had already added the BiPAP back earlier in the day and it wasn’t cutting it. Time to try NAVA (Neurally Adjusted Ventilatory Assist). Basically a more synchronized breath on the ventilator. I was already on my way back to the hospital and told her I would see her soon.
When I arrived I saw people crowded outside and inside his room. The big glass doors were open and the first person I laid eyes on was Cheri, the chaplain. My heart sunk and my eyes started welling up with tears. Dr. Rood, several nurses, respiratory and more were there. They had Finn laid flat and were helping him breathe. It looked bad, the worst I have ever seen him. I could see him wriggling and watched his chest retract. He was grunting with every breath. Dr. Rood informed me that I needed to call Jeff and that he needed to be here because they are taking him into emergency surgery. He was getting his Broviac placed immediately. She felt that he needed intubation to breathe and was not comfortable leaving him overnight without immediate access. An IV wasn’t going to cut it. An anesthesiologist and surgeon were there before I could process what was happening. We started talking risks, bleeding out and ECMO. I told Finn over and over again that I wasn’t done with him yet. That we have too many songs to sing, books to read, zoo trips and playgrounds to visit. That we haven’t even made it to the fun stuff yet so he had to hang on. It’ll be worth it, I promised him. Jeff showed up, we kissed him, loved on him and off to the OR he went.
It’s hard to laugh anymore. Especially here in the hospital. One of the respiratory therapists, Sheri, kept talking about how Finn was being such a buggar. That he was messing with all of our plans and making everyone’s lives a pain in the butt. That he was scaring everyone on the floor. They all adore him so much now and none of them want to see this sort of situation happen. I told her it’s our fault. We called him Danger when he was in the womb and he took me too seriously. They all got a kick out of that. He definitely has lived up to that nickname. They laughed and laughed. Encouraging us to rename him when we come out on the other side of this. Finnegan Danger Olson, or if he keeps pushing it, Finnegan Moore Danger Olson. This made waiting a lot easier. Having a smile with the sweet people who care about him here.
The OR nurse called. They had successfully sedated and intubated him. The scariest part was over. Placing the Broviac is rather routine, but still comes with risks. I was mostly concerned with the initial sedation so my fears had been calmed. The surgery was over before we knew it and they were wheeling our baby back to his new room. Room 8. We are back in the center of the action. Our room is big and right next to the nurses station and doctors’ office again. We were back to full time nursing coverage. This kid likes the attention.
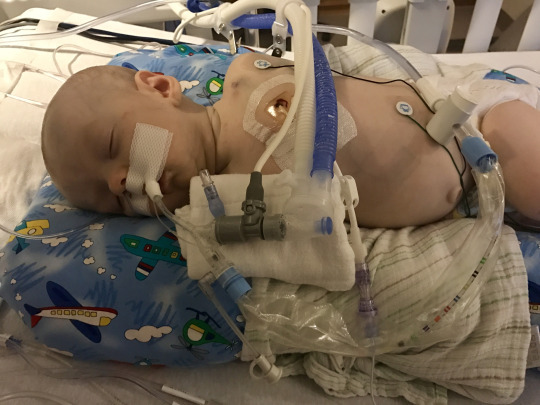
There was a lot of work to get him situated after x-rays and assessments. The hooked up a lot of new IVs to his Broviac line, inserted an arterial line to monitor blood pressures and retaped his breathing tube. It was pretty intense to watch. People kept coming and going, reviewing labs, pulses and looking at the screens. As far as I could tell, he seemed drugged up but comfortable. What do I know? Our evening intensivist called for a transfusion. His hemoglobin was low and he was looking rather pale. He needed the extra blood. I was concerned because we had previously been told that a transfusion could affect his transplant status. Dr. Huntley talked me through it, called Dr. Vezmar and we decided to move forward. He quickly improved and his numbers got better.
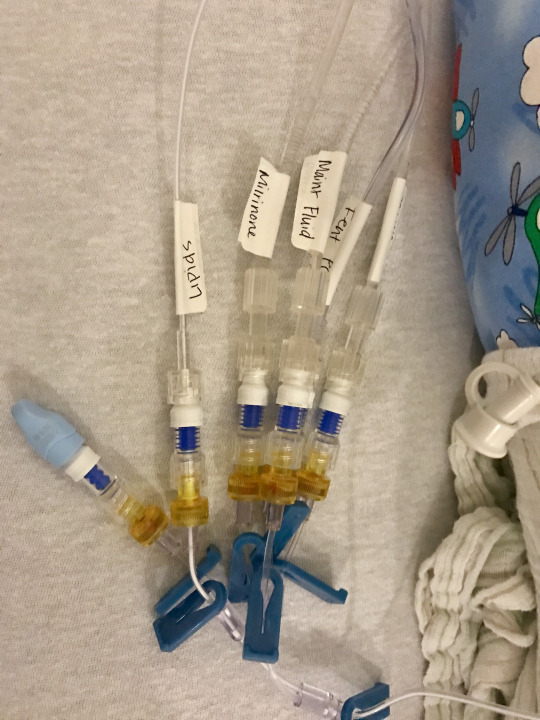
After an uneventful night and morning Finn went in for his scheduled procedure to add a surgical feeding tube. He did well and now he has two after market accessories that we can go home with if needed. These are more permanent solutions to what we had previously been doing. He is going to need access and nutrition throughout the next part of our journey and hopefully this will make it all easier long term.
Speaking of our journey, we have officially received the green light to move to Rochester. Our team said it’s time, especially after the last few days. On Monday, May 1st we will be on the road (literally and figuratively) to listing our sweet Finnegan for a heart transplant. The process should take under two weeks. We expect that by his four month birthday (May 13th) he will be waiting patiently for the gift of life. It’s bittersweet. I don’t want to leave the care we’ve received here. The doctors and nurses have become a family to us. They love our son and we love them. I’m scared. It’s the unknown. Will they love Finn the same way? Will the nurses hold my hand and sit with me when I need things explained for the 5th time? With the doctors hug me when I’m crying? Will they ask how Asher is and care about us as a family? I hope so. I’ve been told it’s a culture shock and that they do things differently down there. They aren’t a children’s hospital with family centered care, but a hospital. A big machine. But, the machine that will save my son’s life.
April 26, 2017

Comments
Post a Comment